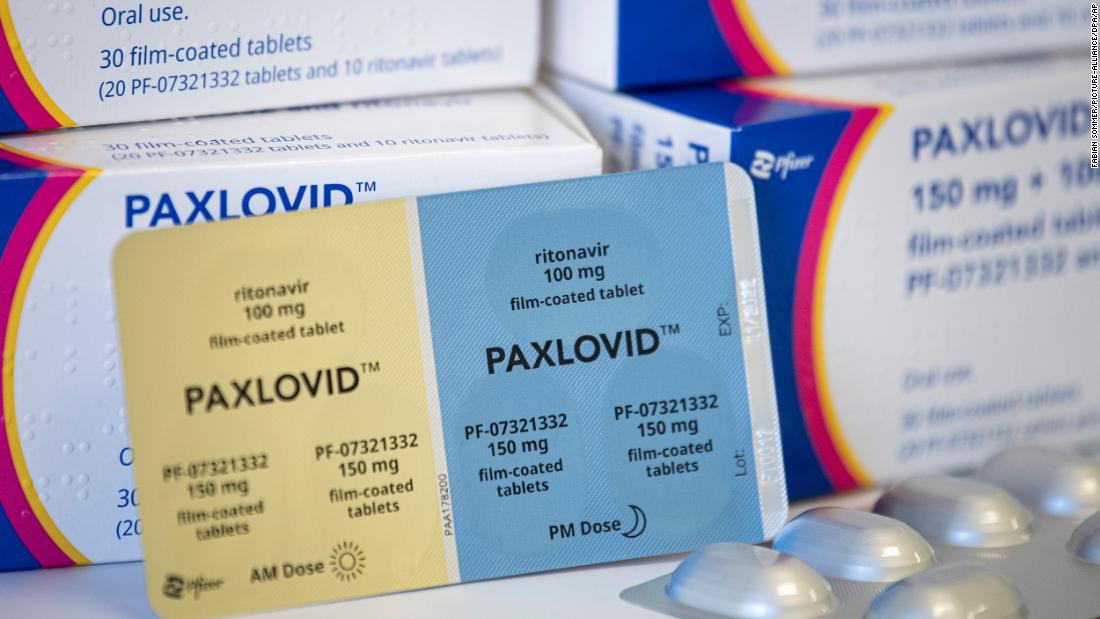
Pharmacists call to Medicare over Pfizer prescribing power
The FDA’s decision to let pharmacists prescribe Pfizer’s Paxlovid could be a game changer in expanding access to Covid-19 treatment, but only if pharmacies receive adequate payment for their work, business groups say.
The Food and Drug Administration announced this week that state-licensed pharmacists can prescribe Pfizer’s Covid pill to eligible patients, with certain limitations. The move drew praise from U.S. pharmacists who for months have called for prescribing changes to rules to facilitate access to rural and minority communities, which often rely on independent pharmacists as their primary source of care.
But pharmacies say they would be better equipped to deal with this new responsibility if the Medicare agency asked health plans to pay them to evaluate patients and do other work needed to dispense the pill.
Some health plans have been handing out just $ 1, the groups say.
“If pharmacies are only paid dispensing fees as they have been, then nothing will improve,” said Kurt Proctor, senior vice president of strategic initiatives for the National Association of Community Pharmacists.
“Hopefully, the other branches of government will follow up on this FDA action and describe how they will pay pharmacists for this activity, and that it will be fair and equitable,” said Proctor, whose organization represents more than 19,000 independent people. pharmacies across the US.
A spokesman for the Medicare and Medicaid Service Centers said in an email that the agency has encouraged health plans to pay an appropriate dispensation fee for those drugs and urged Medicare Part D plans to ensure I know that eligible patients can easily access treatment if they need it. that.
The spokesman added that the agency may update its guidelines for Part D plan sponsors in the future.
The FDA said on July 6 that patients seeking Paxlovid should bring a full list of medications so the pharmacist can review possible drug interactions, as well as a result of the last 12 months’ blood test. Pharmacists should refer patients to a doctor or other primary care provider if the patient’s existing medication list needs to be changed or if there are questions about their kidney or liver function, the agency said.
“Since Paxlovid should be taken within five days of the onset of symptoms, authorizing state-licensed pharmacists to prescribe Paxlovid could expand access to timely treatment for some patients who are eligible to receive this medication for to the treatment of COVID-19 “, Patrizia Cavazzoni, director. of the FDA’s Drug Evaluation and Research Center said in a statement.
Improving equity
Pharmacists say allowing them to prescribe will alleviate some barriers that have so far limited the scope of the Biden administration’s Covid treatment initiatives.
President Joe Biden unveiled his Test to Treat initiative earlier this year, which now has thousands of locations across the country where patients can immediately receive an authorized antiviral pill from Pfizer or Merck & Co. if they give positive.
These sites have been created in pharmacy clinics, community health centers, and other facilities that have in-house physicians or other licensed prescribers. Pharmacy groups say minority and rural communities often have difficulty accessing these places, which further exacerbated health inequalities exacerbated by the Covid-19 pandemic.
“Opening the door to pharmacists as prescribers will open the door to equitable access to pharmacies in communities across the country,” said Ilisa Bernstein, interim executive vice president and CEO of the American Association of Pharmacists.
Tom Kraus, vice president of government relations for the American Society of Health-System Pharmacists, said the group was “delighted to see the FDA remove this barrier to patients’ access to this critical treatment.”
“Pharmacists have played a vital role in our pandemic response efforts and are well positioned to help patients, especially those in rural and disadvantaged communities, benefit from this drug,” he added.
Medicare action
Demands from pharmacists to be able to prescribe increased after high-risk Americans reported having difficulty getting Covid-19 antiviral pills while prescribers struggled with limited guidance.
Pharmacists say the change will be more likely to successfully improve health equity if health plans reimburse them properly.
Right now, a pharmacist can take up to 30 minutes to evaluate a patient to determine if Paxlovid is right for them and also identify any drug interactions, Bernstein said.
“It is important that CMS and other payers develop payment channels to reimburse pharmacists for their services related to patient assessment and prescription of the drug, just as it is paid to any other prescriber,” he said.
The CMS said in November 2021 that while some antiviral drugs would initially be available at no cost to pharmacies, typical dispensing fees would not be covered automatically. The agency said it “strongly encourages” sponsors of Medicare Part D prescription drug plans to pay these fees, but did not suggest an amount.
The NCPA said in a January letter to the CMS that health insurance plans were paying up to $ 10.50 for the dispensation fee, an amount that, according to the group, should approach $ 40. which requires Medicare to cover a single dose of Covid-19 vaccine.
Pharmacists now looking to prescribe Paxlovid directly to patients will have to work even harder in addition to dispensing tasks to get Paxlovid to patients who need it, Proctor said.
“I expect Medicare and CMS and other payers to pay for this professional service,” he added.
Congress
Congress should also join the push for adequate Medicare coverage of pharmacy services, the National Drug Chain Association said.
A bill in the House (HR 7213) from Rep. Ron Kind (D-Wis.) Would provide Medicare Part B coverage for pharmaceutical services, including treatment for conditions like Covid-19. The measure was introduced in March and has not yet advanced.
Steven C. Anderson, president and CEO of NACDS, said the FDA’s prescription order change was “a crucial step forward” that should drive others to act.
“We encourage the federal government to take the next necessary steps to support pharmacy-based assessments that guide the use of this life-saving therapy,” he said.

Comments are closed.